Minimally invasive non-surgical therapy (MINST) for patients with intraosseous defects is aimed at minimizing tissue trauma and accelerating wound healing by eliminating surgical incisions and sutures.
Despite improvements in treatment methods, intraosseous defects are associated with the progression of periodontal disease and tooth loss if not treated with complex surgical interventions. Now, in a first-of-its-kind multicentre study, scientists from the Faculty of Dentistry and Maxillofacial Sciences at King's College London have analyzed the clinical and radiological results of non-surgical treatment of intraosseous defects and have concluded that it is a viable treatment option.
Despite its successes, regenerative surgery often involves pain, complications and high financial costs. Results are not always predictable and clinical failures and limited success have been reported. Minimally invasive non-surgical therapy (MINST) is a shift towards more patient-friendly alternatives. This approach aims to minimize tissue trauma and accelerate wound healing by eliminating surgical incisions and sutures. But because the predictability, generalizability, and broad application of MINST remain unclear, the research team's goal was to evaluate the effect of MINST on intraosseous defects.
The study analyzed data from 48 patients with one or more intraosseous defects who were treated in private practice in the UK, Italy and Spain. Patients received stage 1 and stage 2 periodontal therapy, including MINST. Clinical and periapical radiographic findings were analyzed at baseline and 12 months thereafter.
The average total depth of the defect on the radiograph decreased by 1.42 mm, and the angle of the defect increased by 3°. Statistically significant improvements in probing pocket depth (PPD) and clinical attachment level (CAL) at 12 months were compared with baseline. In 66.7%, a probing pocket depth of 4 mm or less was achieved, and in 58.3% of defects, the clinical level of attachment increased by 3 mm. Deeper and narrower defects showed significant radiographic and clinical improvements, respectively.
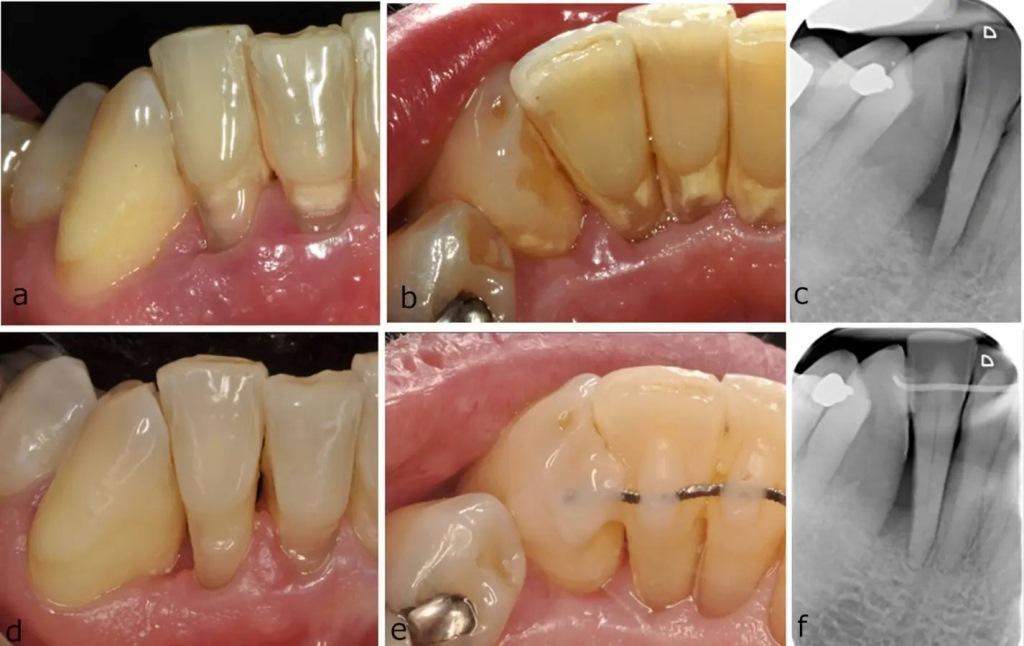
Figure 1: Baseline photographs (a–c) and clinical photographs and 12-month radiographs (d–f) of a distal intraosseous defect of a right mandibular lateral incisor. After minimally invasive non-surgical treatment and splinting, the depth of the probing pocket on the distobuccal side of the right mandibular lateral incisor decreased from 12 mm to 3 mm.
“These results are consistent with those reported in previous single-center MINST studies and provide further evidence that an atraumatic technique that minimizes tissue damage and trauma while increasing gingival margin stability and reducing chair time can significantly improve intraosseous defects,” the study authors said. However, they emphasized that to achieve the clinical goal of an increase in PPD of less than 5 mm and no bleeding on probing, surgery may be required in some cases.
The researchers said the main limitations of this study were the lack of a control group, the exclusion of smokers, which limited the generalizability of the results, and the use of non-standardized radiographs.
“The study results demonstrate the feasibility of this method as a potential method of saving many teeth with advanced gum problems without the need for surgery,” study co-author Dr. Luigi Nibali, professor of periodontology at Queen's Medical University, said in a press release. “This has the potential to reduce NHS and patient costs and of course the treatment will be much more convenient for the patient,” he added.
The study authors emphasized that MINST should be considered a viable treatment approach and that its effectiveness should be confirmed in the form of further controlled multicenter studies.
